 
Braun Medical Inc., Bethlehem, PA) (Figure 2A, ,2B). VERAFLO™ Instillation Therapy (Kinetic Concepts, Acelity, San Antonio, TX) was performed on the right forearm with wound vac settings set to -125 mmHg suction and instillation of Prontosan® Wound Irrigation Solution (B. Application of a circumferential NPWTi-d using V.A.C. Clearly nonviable eschar was debrided, but any tissue with questionable viability was left alone. We performed minimal debridement of the skin, muscle, and fascia. Dusky muscle was again noted at the proximal aspects of both dorsal and volar compartments, which was minimally responsive to electrocautery stimulation. 
The patient was taken to the OR after admittance to the hospital for irrigation/debridement and reassessment of the right forearm. Intravenous fluids were started for kidney protection and CK clearance, and IV cefazolin was continued. Second look to ensure adequate release of forearm compartments, and repeat irrigation and debridement was indicated and would be performed as soon as possible. The decision was made to admit the patient to the pediatric intensive care unit for hourly monitoring until surgery could be performed. Mild anemia was noted with hemoglobin level of 9, but without associated systemic or clinical symptoms, and therefore treatment was not indicated. Baseline electrolytes were within normal limits. 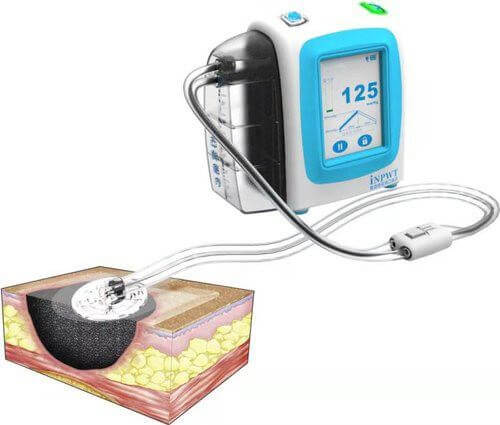
Laboratory work-up revealed creatine-kinase (CK) level of over 13,086 with no evidence of impaired renal function. At-risk and dusky skin is noted radially. (A) Volar forearm fasciotomy site with myonecrosis noted proximally. Initial presentation of right forearm fasciotomy wounds Dusky muscle was noted at the proximal aspect of the volar and dorsal compartments (Figure (Figure1A, 1A, ,1B 1B]. Skin on the radial volar surface of the forearm presented with duskiness and surrounding erythema. Volar and dorsal fasciotomy sites were clean without evidence of gross infection. The patient had no spontaneous movements of the right wrist or fingers and did not respond to touch. The comprehensive history and physical was unremarkable for new findings and was consistent with the previous findings prior to transfer in regards to the right upper extremity. Focused physical examination of the right upper extremity revealed persistent motor and sensory deficits of the median, radial, and ulnar nerves at the level of the wrist and fingers. Our patient was then seen in the emergency room at our facility where a repeat history and physical was performed. The patient subsequently underwent volar and dorsal forearm fasciotomies where questionably viable muscle was reported. He was started on intravenous cefazolin, and subsequently transferred to the pediatric hospital for definitive management. The diagnosis was confirmed with intracompartmental pressure readings. He was taken back to the hospital where compartment syndrome was suspected. Additionally, she noticed the patient was no longer moving his hand, and he was unresponsive to touch along his fingers. Over the course of two days, the patient’s mother reported the patient's complaints of pain became progressive. The injury was successfully closed reduced and splinted without complication. He was diagnosed with a right both bone forearm fracture (BBFF), which includes the radius and ulna bones. Our patient is a three-year-old boy who presented to an outside hospital after jumping and falling from a couch thus sustaining a right forearm injury. We present a case report on the novel use of circumferentially applied negative pressure wound therapy with instillation and dwell (NPWTi-d) followed by circumferentially applied closed-incision negative pressure therapy (ciNPWT) for the management of a complex fasciotomy wound in a pediatric patient. Previous studies indicate negative pressure wound therapy (NPWT) has beneficial effects on fasciotomy wound healing by reducing time to closure in adults however, there is a paucity of literature on the utility of NPWT in managing pediatric ACS. Appropriate wound management is therefore needed to minimize potential complications and morbidity. Gold standard treatment for pediatric compartment syndrome is fasciotomies, which are associated with extended hospital stay, infection, and secondary soft tissue procedures such as primary closure and grafting procedures. Significant delays in treatment of ACS in pediatric patients are associated with permanent disability, flail limb, and/or need for amputations. An unreliable physical exam and communication barrier are some of the challenges encountered with pediatric patients (especially with children 24 hours). 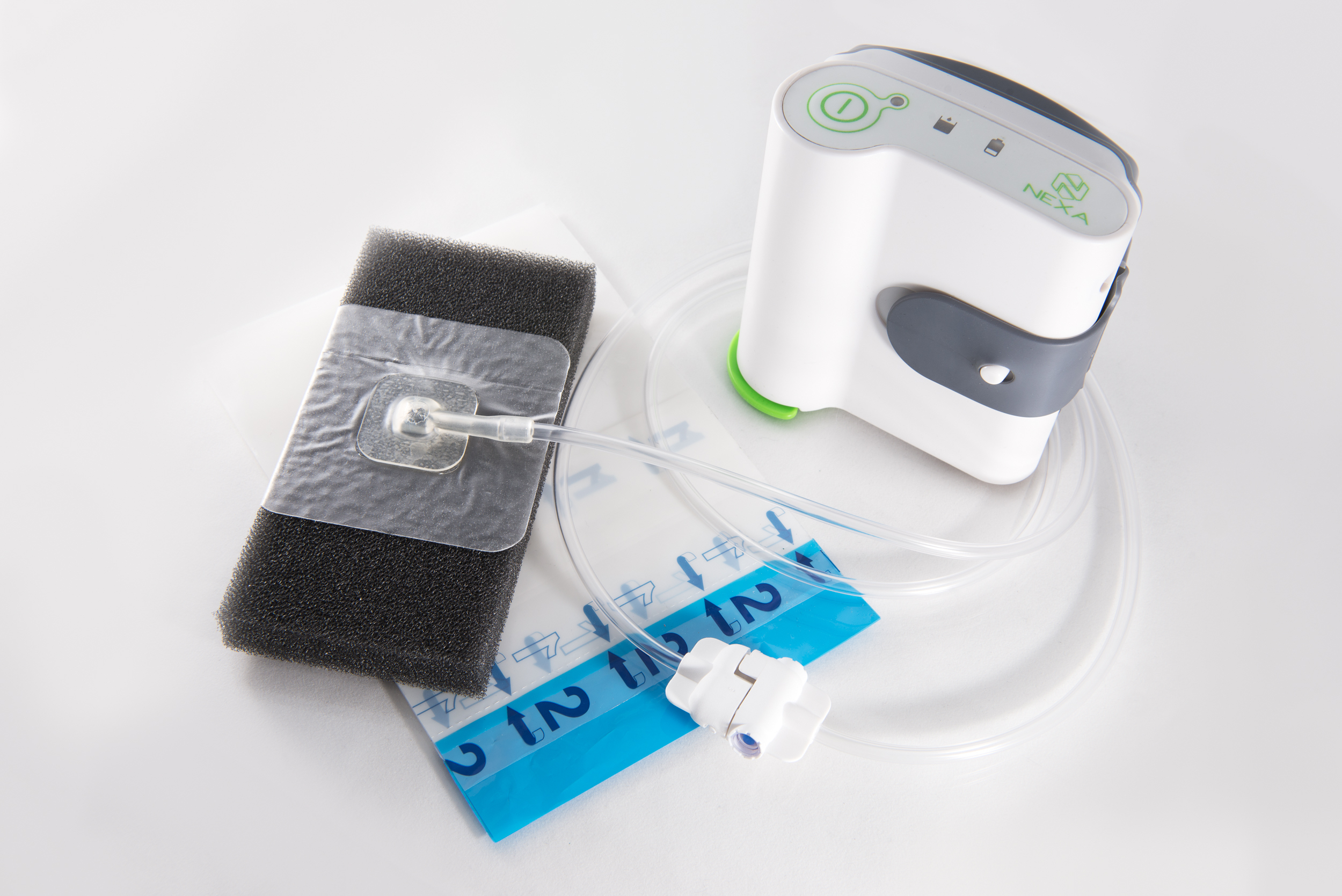
Children pose unique challenges in identification and management of compartment syndrome. Acute compartment syndrome (ACS) in the pediatric population is a rare orthopaedic emergency with potentially devastating consequences if not treated appropriately. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
